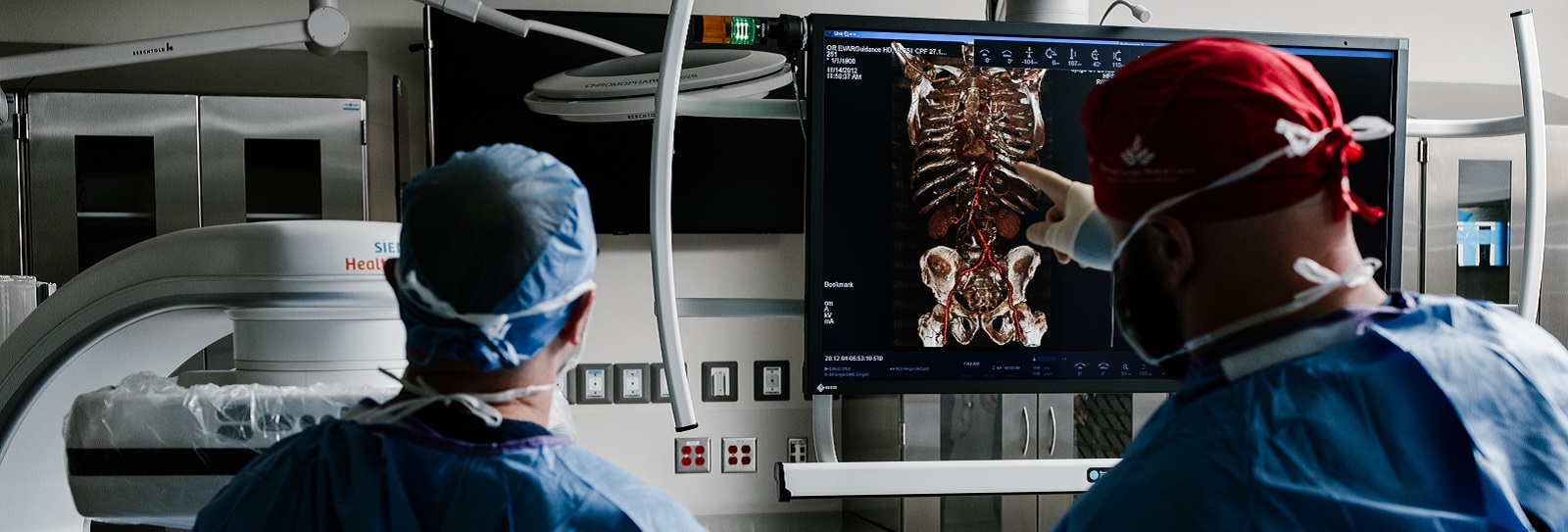
NGMC Gainesville is home to two endovascular operating rooms (EVOR), both of which has been fully updated to have the most innovative technology and equipment available.
As a type of specialized operating room, an EVOR has enhanced capabilities, including catheterization and imaging technologies, both of which are used to perform minimally-invasive or endovascular procedures.
“The new EVOR is another example of how NGMC is setting the standard for vascular care in Northeast Georgia. It utilizes state-of-the-art surgical equipment, along with advanced imaging technology, so that we can quickly and efficiently perform the complete spectrum of vascular procedures, from traditional, open surgery to minimally-invasive, image-guided procedures. And we’re doing it faster and more precisely than ever before.”
James Reeves, MD, Northeast Georgia Physicians Group (NGPG) vascular surgeon, medical director of the EVOR
Features of the New EVOR
As an operating room equipped with world-class technology and equipment, NGMC’s new EVOR has several key features. Most notably is the addition of the ARTIS pheno, an advanced interventional angiography system. This technology helps to streamline care, expand services and simplify even the most complex procedures.
In addition to the ARTIS pheno, the new EVOR is also equipped with all of the resources and equipment necessary to perform traditional, open surgery.
This means that any type of advanced vascular intervention can be safely and effectively performed without having to move the patient. This includes surgical treatment of thoracic and abdominal aortic aneurysms, aortic dissection and peripheral artery disease.
The EVOR may also be used for treatment of traumatic injuries, such as thoracic tears, which is an injury that can result from the impact in a motor vehicle or motorcycle crash.


EVOR Benefits
For more than a decade, the vascular surgeons of NGPG and Longstreet Clinic have utilized NGMC’s existing EVOR to perform thousands of minimally-invasive procedures every year.
The new EVOR features state-of-the-art technology and provides several additional benefits, such as:
- Increased Capacity: Procedures are performed faster and more efficiently, meaning that NGMC can care for even more vascular patients.
- Faster Procedures: The full range of endovascular services can be provided faster and with greater precision, which gets patients treated and into recovery as quickly as possible.
- Expanded Capabilities: Even the most complex procedures can be treated in a fraction of the time and without transferring patients to other hospitals.
Endovascular Experts
The staffing of the endovascular suite is perhaps the most important aspect of the room. Because vascular surgery combines multiple modalities of care, the staff is cross-trained to meet any demands that arise while performing endovascular procedures.
In addition to the dedicated and specialty-trained EVOR clinical team, the vascular surgeons of NGPG and Longstreet Clinic have years of experience and are leaders in the field of endovascular surgery. With this exceptional team of experts and a new state-of-the-art EVOR, NGMC is equipped to provide every type of endovascular procedure – and more.
“We have assembled a team of experts from cardiology, surgery and interventional radiology to provide a collaborative and unrivaled level of care to patients in need of endovascular treatment and services. Plus, this expert team is always available, 24 hours a day, 7 days a week, to ensure that emergent vascular cases are rapidly treated. If a patient comes in with a ruptured aneurysm, for example — meaning they have lost circulation to their lower leg — we are always ready to provide care as quickly as possible.”
James Reeves, MD, Northeast Georgia Physicians Group (NGPG) vascular surgeon, medical director of the EVOR